Selecting a topic
When looking at a number of potential topics I wanted to select a topic that I was passionate about and that had a reliable date/ multiple reliable datasets I could draw from. Of the topics I reviewed, I decided to focus on mental health statistics as this is an area of interest to me and an area of growing concern due to the impact of COVID-19 on mental health services on a global scale.
Population-based mental health statistics
Source: https://ourworldindata.org/mental-health
I began my research by looking at the world statistics on mental health on Our World in Data. It is clear that there are some issues around the accuracy of the data as mental health is widely under-reported across all countries however particularly in lower-income countries. The statistics I have included below were published in 2018 and only cover up to 2017.
In 2017 it is estimated that 729 million people lived with a global mental health disorder (just over 1 in 10 globally 10.7%). Below is a table providing a breakdown of these results splitting mental health disorders into 10 categories: Depression, Anxiety disorder, Bipolar disorder, Eating disorders, Schizophrenia, Any mental or substance use disorder, Alcohol use disorder and Drug use disorder (excluding alcohol)
This provides a good overview of the most current global statistics on the subject breaking the number of people who have been recorded as having one of the above mental health disorders across the world population as a percentage and number as well as breaking the number down further my gender.
These statistics are then broken down by disorder are provided by location, across a timespan (1990-2017) and by gender. More general information is also supplied about what the disorder is the different forms it comes in.
Depression
Depressive disorders range within severity from mild persistent depression to major depressive disorder. All forms of depressive disorder experience some of the below symptoms as outlined on our world in data:
-
reduced concentration and attention;
-
reduced self-esteem and self-confidence;
-
ideas of guilt and unworthiness (even in a mild type of episode);
-
bleak and pessimistic views of the future;
-
ideas or acts of self-harm or suicide;
-
disturbed sleep
-
diminished appetite.
Anxiety disorder
Anxiety disorders come in different forms including phobic, social, obsessive-compulsive (OCD), post-traumatic disorder (PTSD), or generalized anxiety disorders. Below are common symptoms that are present across most forms of anxiety disorder as outlined by WHO:
-
apprehension (worries about future misfortunes, feeling “on edge”, difficulty in concentrating, etc.);
-
motor tension (restless fidgeting, tension headaches, trembling, inability to relax);
-
autonomic overactivity (lightheadedness, sweating, tachycardia or tachypnoea, epigastric discomfort, dizziness, dry mouth, etc.).”
Bipolar disorder
Below is WHO’s definition of Bipolar disorder:
“This disorder is characterized by repeated (i.e. at least two) episodes in which the patient’s mood and activity levels are significantly disturbed, this disturbance consisting on some occasions of an elevation of mood and increased energy and activity (mania or hypomania), and on others of a lowering of mood and decreased energy and activity (depression). Characteristically, recovery is usually complete between episodes, and the incidence in the two sexes is more nearly equal than in other mood disorders. As patients who suffer only from repeated episodes of mania are comparatively rare, and resemble (in their family history, premorbid personality, age of onset, and long-term prognosis) those who also have at least occasional episodes of depression, such patients are classified as bipolar.”
Eating disorders
Eating disorders are considered to be psychiatric condition defined by patterns of disordered eating. Eating disorders incorporate a spectrum of disordered eating behaviours. The data found above only present data the disorders of anorexia and bulimia nervosa.
Anorexia nervosa: “Anorexia nervosa is a disorder exemplified by deliberate weight loss, and associated with undernutrition of varying severity.”
Bulimia nervosa: “Bulimia nervosa is an illness defined by repeated behaviours of overeating, preoccupation with control of body weight, and the adoption of extreme measures to mitigate the impacts of overeating”
Schizophrenia
Below is NHS’s overview of schizophrenia and it’s symptoms:
Doctors often describe schizophrenia as a type of psychosis. This means the person may not always be able to distinguish their own thoughts and ideas from reality.
Symptoms of schizophrenia include:
- hallucinations – hearing or seeing things that do not exist outside of the mind
- delusions – unusual beliefs not based on reality
- muddled thoughts based on hallucinations or delusions
- losing interest in everyday activities
- not caring about your personal hygiene
- wanting to avoid people, including friends
Schizophrenia does not cause someone to be violent and people with schizophrenia do not have a split personality.
https://www.nhs.uk/mental-health/conditions/schizophrenia/overview/
Mental Health as a risk factor for substance abuse
Mental health is known to be an important risk factor for the development of substance use disorders (either in the form of alcohol or illicit drug dependencies). The increased risk of a substance use disorder varies by mental health disorder type:
alcohol dependency the risk is highest in individuals with intermittent explosive disorder, dysthymia, ODD, bipolar disorder and social phobia. This is discussed in our entry on Alcohol Consumption.
illicit drug dependency the risk is highest for individuals with intermittent explosive disorder, ADHD, and bipolar disorder. This is discussed in our entry on Substance Use.
Mental health and suicide
Studies of suicide across high-income countries suggests that 90% are a result of an underlying mental health or substance use disorder. In a study by Ferrari et al. (2015) only 68% of suicides across China, Taiwan and India were attributed to mental health and substance use disorders. In these instances, a large number of suicides result from the ‘dysphoric affect’ and ‘impulsivity’, these are not defined as mental and substance use disorders.
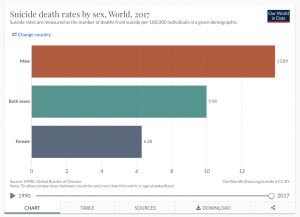
Suicide Rates
https://ourworldindata.org/suicide#share-of-deaths-from-suicide
Globally 1.4 % of deaths were from suicide in 2017.
Word suicide rates by age and gender:
It may be helpful to provide additional information on suicide and suicide rates to add context to the impact of mental health on suicide e.g. which age group and gender are most affected and the amount of death accounted for are as a result of suicide- it will be important for me to highlight at this stage that these statistics are pre-covid.
Statistics I would like to include in my infographic
Below are various facts and statics I have pulled directly from a number of sources that I would like to include in my infographic
- It is estimated that 792 million people live with a mental health disorder just over one in 10 (10.7%)
- Share of the global population with disorders (disorders are broken into 10 categories)- bar chart
- World distribution of mental and substance disorders- map
- In high-income countries, meta-analyses suggest that up to 90% of suicide deaths result from underlying mental and substance use disorders.- could maybe include map of high-income countries- the list is quite long
- 68 percent of suicides across China, Taiwan and India were attributed to mental health and substance use disorders. Here, studies suggest a large number of suicides result from the ‘dysphoric affect’ and ‘impulsivity’ (which are not defined as a mental and substance use disorder) Ferrari et al. (2015)
- Studies suggest that for an individual with depression the risk of suicide is around 20 times higher than an individual without.
- Mental ill-health is the single largest cause of disability in the UK, contributing up to 22.8% of the total burden, compared to 15.9% for cancer and 16.2% for cardiovascular disease. The wider economic costs of mental illness in England have been estimated at £105.2 billion each year. This includes direct costs of services, lost productivity at work and reduced quality of life (https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/215808/dh_123993.pdf)
- A recent WHO-led study estimates that depression and anxiety disorders cost the global economy US$ 1 trillion each year in lost productivity. For every US$ 1 put into scaled up treatment for common mental disorders, there is a return of US$ 4 in improved health and productivity. https://www.who.int/teams/mental-health-and-substance-use/mental-health-in-the-workplace
-
Based on data from 2010, the global direct and indirect economic costs of mental disorders were estimated at US$2.5 trillion. Importantly, the indirect costs (US$1.7 trillion) are much higher than the direct costs (US$0.8 trillion), which contrasts with other key disease groups, such as cardiovascular diseases and cancer. For the EU, a region with highly developed healthcare systems, the direct and indirect costs were estimated at €798 billion 7. Both direct and indirect costs of mental disorders are expected to double by 2030 (Fig 2A). It should be noted that these calculations did not include costs associated with mental disorders from outside the healthcare system, such as legal costs caused by illicit drug abuse. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5007565/ – might be nice to have a representation of 100k, million, billion, trillion to make the point https://johntreadgold.com/blog/million-vs-billion-vs-trillion/
- Percentage of people with common mental health problems receiving treatment in 2000, 2007 and 2014- https://www.mentalhealth.org.uk/statistics/mental-health-statistics-people-seeking-help bar chart in the UK
- Prevalence rates in males and female by mental health disorder across the word https://ourworldindata.org/mental-health#deaths-from-mental-health-and-substance-use-disorders
- The COVID-19 pandemic has disrupted or halted critical mental health services in 93% of countries worldwide while the demand for mental health is increasing
- prior to the pandemic, countries were spending less than 2 per cent of their national health budgets on mental health, and struggling to meet their populations’ needs.
- Over 60% reported disruptions to mental health services for vulnerable people, including children and adolescents (72%), older adults (70%), and women requiring antenatal or postnatal services (61%).
- 67% saw disruptions to counselling and psychotherapy; 65% to critical harm reduction services; and 45% to opioid agonist maintenance treatment for opioid dependence.
- More than a third (35%) reported disruptions to emergency interventions, including those for people experiencing prolonged seizures; severe substance use withdrawal syndromes; and delirium, often a sign of a serious underlying medical condition.
- 30% reported disruptions to access for medications for mental, neurological and substance use disorders.
- Around three-quarters reported at least partial disruptions to school and workplace mental health services (78% and 75% respectively). https://www.who.int/news/item/05-10-2020-covid-19-disrupting-mental-health-services-in-most-countries-who-survey
- A significant proportion of patients self-rated in the psychopathological range: 28% for PTSD, 31% for depression, 42% for anxiety, 20% for OC symptoms, and 40% for insomnia. Overall, 56% scored in the pathological range in at least one clinical dimension. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7390748/